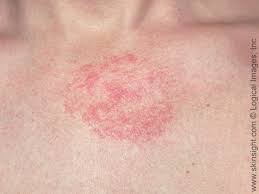
FDA approves dupilumab for moderate to severe eczema
“Sanofi and Regeneron Pharmaceuticals, Inc. announced today that the U.S. Food and Drug Administration (FDA) approved Dupixent® (dupilumab) Injection, the first and only biologic medicine approved for the treatment of adults with moderate-to-severe atopic dermatitis… Read More »FDA approves dupilumab for moderate to severe eczema